The Best Yeast Infection Pills, Creams, and Treatment Options
Dealing with a yeast infection can be uncomfortable and frustrating, but there are many effective treatment options available, including pills, creams, and home remedies. Here’s a comprehensive guide to the best yeast infection treatments to help you find relief and restore balance.
What is a Yeast Infection?
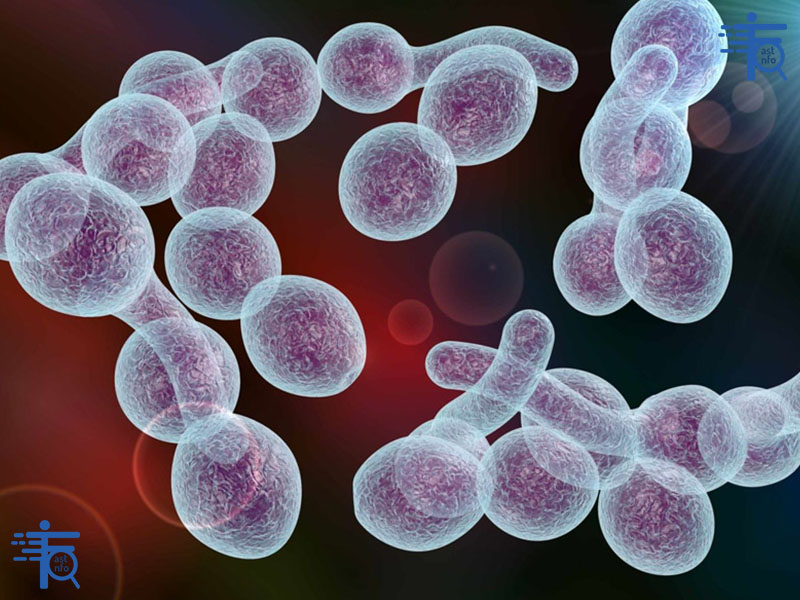
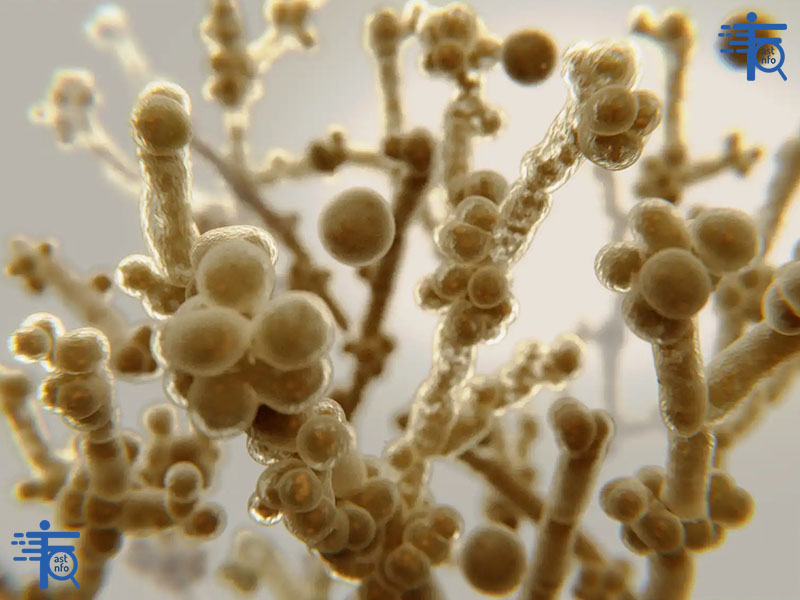
A yeast infection (candidiasis) is caused by an overgrowth of the fungus Candida albicans. It commonly affects the vaginal area but can also occur in the mouth (thrush), skin, or other parts of the body. Symptoms include itching, burning, redness, and discharge.
Best Yeast Infection Treatments
1. Over-the-Counter (OTC) Antifungal Creams
OTC creams are a popular and effective first-line treatment for yeast infections. They contain antifungal ingredients like clotrimazole, miconazole, or tioconazole.
- Top Picks:
- Monistat (Miconazole): Available in 1-day, 3-day, and 7-day treatments.
- Clotrimazole (Gyne-Lotrimin): A gentle option for sensitive skin.
- Tioconazole (Vagistat): A single-dose treatment for quick relief.
- How to Use: Apply the cream directly to the affected area as directed. Most treatments provide relief within a few days.
2. Antifungal Pills
Oral antifungal medications are prescribed for severe or recurrent yeast infections. They work systemically to eliminate the infection from within.
- Top Picks:
- Fluconazole (Diflucan): A single-dose pill that’s highly effective.
- Itraconazole: Used for more resistant or systemic yeast infections.
- How to Use: Take the pill as prescribed by your healthcare provider. Fluconazole is often taken as a one-time dose, but recurrent infections may require multiple doses.
3. Prescription Vaginal Creams
For stubborn or recurrent infections, your doctor may prescribe stronger antifungal creams.
- Top Picks:
- Terconazole (Terazol): A prescription-strength cream for severe infections.
- Nystatin: Often used for oral thrush or skin yeast infections.
- How to Use: Apply the cream as directed by your healthcare provider, usually for 7–14 days.
4. Probiotics
Probiotics help restore the balance of good bacteria in the body, which can prevent and treat yeast infections.
- Top Picks:
- Lactobacillus rhamnosus and Lactobacillus reuteri: Strains specifically beneficial for vaginal health.
- Oral Probiotic Supplements: Look for brands like Culturelle or Renew Life.
- Vaginal Probiotic Supplements: Products like Fem-Dophilus or RepHresh Pro-B.
- How to Use: Take daily as a supplement or use vaginal probiotic suppositories.
5. Home Remedies
For mild infections or as a complementary treatment, some home remedies can provide relief.
- Top Picks:
- Yogurt: Plain, unsweetened yogurt with live cultures can be applied topically or consumed to promote healthy bacteria.
- Coconut Oil: Contains caprylic acid, which has antifungal properties. Apply topically to the affected area.
- Apple Cider Vinegar: Dilute with water and use as a soak or rinse to restore pH balance.
- Garlic: Contains allicin, a natural antifungal. Insert a peeled garlic clove (wrapped in gauze) vaginally overnight.
- How to Use: Use these remedies with caution and discontinue if irritation occurs.
How to Choose the Right Treatment
- Severity of Symptoms: Mild infections can often be treated with OTC creams, while severe or recurrent infections may require prescription pills or creams.
- Convenience: Pills like fluconazole offer a one-dose solution, while creams may require multiple applications.
- Personal Preference: Some people prefer oral medications, while others find topical treatments more soothing.
- Underlying Health Conditions: If you have diabetes, a weakened immune system, or are pregnant, consult your doctor before starting any treatment.
Preventing Yeast Infections
- Practice Good Hygiene: Keep the genital area clean and dry.
- Avoid Irritants: Steer clear of scented products, douches, or tight-fitting clothing.
- Wear Breathable Fabrics: Choose cotton underwear and avoid synthetic materials.
- Maintain a Healthy Diet: Limit sugar and refined carbs, which can feed yeast.
- Take Probiotics: Regularly consume probiotic-rich foods or supplements to support healthy bacteria.
When to See a Doctor
- If symptoms persist after treatment.
- If you experience recurrent yeast infections (more than 4 per year).
- If you’re pregnant or have underlying health conditions.
- If you’re unsure whether your symptoms are due to a yeast infection or another condition (e.g., bacterial vaginosis or a sexually transmitted infection).
How are yeast infections treated?
Yeast infections, caused by an overgrowth of the fungus Candida albicans, are commonly treated with antifungal medications. The treatment approach depends on the severity of the infection, the area affected, and individual health factors. Here’s a detailed guide on how yeast infections are treated:
1. Over-the-Counter (OTC) Treatments
For mild to moderate yeast infections, OTC antifungal medications are often the first line of treatment. These are available in various forms, including creams, ointments, and suppositories.
- Common Active Ingredients:
- Clotrimazole
- Miconazole
- Tioconazole
- Popular Products:
- Monistat (Miconazole): Available in 1-day, 3-day, and 7-day treatments.
- Gyne-Lotrimin (Clotrimazole): A gentle option for sensitive skin.
- Vagistat (Tioconazole): A single-dose treatment for quick relief.
- How to Use:
- Apply the cream or insert the suppository as directed on the packaging.
- Most treatments provide relief within a few days, but it’s important to complete the full course to prevent recurrence.
2. Prescription Medications
For severe, recurrent, or complicated yeast infections, prescription medications may be necessary. These include stronger antifungal creams, oral medications, or longer treatment courses.
- Oral Antifungal Pills:
- Fluconazole (Diflucan): A single-dose pill that’s highly effective for vaginal yeast infections.
- Itraconazole: Used for more resistant or systemic yeast infections.
- Prescription Vaginal Creams:
- Terconazole (Terazol): A stronger antifungal cream for severe infections.
- Nystatin: Often used for oral thrush or skin yeast infections.
- How to Use:
- Take oral medications as prescribed by your healthcare provider.
- Apply prescription creams or suppositories as directed, usually for 7–14 days.
3. Probiotics
Probiotics help restore the balance of good bacteria in the body, which can prevent and treat yeast infections.
- Types of Probiotics:
- Lactobacillus rhamnosus and Lactobacillus reuteri: Strains specifically beneficial for vaginal health.
- Oral Probiotic Supplements: Look for brands like Culturelle or Renew Life.
- Vaginal Probiotic Suppositories: Products like Fem-Dophilus or RepHresh Pro-B.
- How to Use:
- Take daily as a supplement or use vaginal probiotic suppositories.
4. Home Remedies
For mild infections or as a complementary treatment, some home remedies can provide relief. However, these should not replace medical treatment for severe or recurrent infections.
- Common Home Remedies:
- Yogurt: Plain, unsweetened yogurt with live cultures can be applied topically or consumed to promote healthy bacteria.
- Coconut Oil: Contains caprylic acid, which has antifungal properties. Apply topically to the affected area.
- Apple Cider Vinegar: Dilute with water and use as a soak or rinse to restore pH balance.
- Garlic: Contains allicin, a natural antifungal. Insert a peeled garlic clove (wrapped in gauze) vaginally overnight.
- How to Use:
- Use these remedies with caution and discontinue if irritation occurs.
5. Lifestyle and Preventive Measures
Preventing yeast infections is key, especially for those prone to recurrent infections.
- Practice Good Hygiene: Keep the genital area clean and dry.
- Avoid Irritants: Steer clear of scented products, douches, or tight-fitting clothing.
- Wear Breathable Fabrics: Choose cotton underwear and avoid synthetic materials.
- Maintain a Healthy Diet: Limit sugar and refined carbs, which can feed yeast.
- Stay Hydrated: Drink plenty of water to support overall health.
When to See a Doctor
- If symptoms persist after treatment.
- If you experience recurrent yeast infections (more than 4 per year).
- If you’re pregnant or have underlying health conditions (e.g., diabetes, a weakened immune system).
- If you’re unsure whether your symptoms are due to a yeast infection or another condition (e.g., bacterial vaginosis or a sexually transmitted infection).

How do yeast infection treatments work?
Yeast infection treatments work by targeting the overgrowth of Candida albicans, the fungus responsible for most yeast infections. These treatments aim to eliminate the fungus, relieve symptoms, and restore the natural balance of bacteria and yeast in the affected area. Here’s a detailed explanation of how different types of yeast infection treatments work:
1. Antifungal Medications
Antifungal medications are the most common and effective treatments for yeast infections. They work by disrupting the cell walls of the fungus, killing it or preventing its growth.
Types of Antifungals:
- Azoles:
- Examples: Clotrimazole, Miconazole, Fluconazole.
- How They Work: Azoles inhibit the production of ergosterol, a key component of fungal cell membranes. Without ergosterol, the cell membrane becomes leaky and the fungus dies.
- Forms: Creams, ointments, suppositories, and oral pills.
- Polyenes:
- Example: Nystatin.
- How They Work: Polyenes bind to ergosterol in the fungal cell membrane, creating pores that cause the cell to leak and die.
- Forms: Creams, ointments, and oral suspensions (often used for oral thrush).
- Echinocandins:
- Example: Caspofungin.
- How They Work: Echinocandins inhibit the synthesis of beta-glucan, a component of the fungal cell wall, leading to cell death.
- Forms: Typically used for systemic yeast infections in hospitalized patients.
2. Probiotics
Probiotics help restore the natural balance of bacteria and yeast in the body, particularly in the vaginal and gastrointestinal tracts.
How They Work:
- Restore Good Bacteria: Probiotics introduce beneficial bacteria (e.g., Lactobacillus) that compete with Candida for resources, preventing its overgrowth.
- Maintain pH Balance: Beneficial bacteria produce lactic acid, which helps maintain an acidic environment in the vagina, inhibiting yeast growth.
- Boost Immune Response: Probiotics can enhance the body’s immune response to fungal infections.
Forms:
- Oral supplements.
- Vaginal suppositories.
- Probiotic-rich foods (e.g., yogurt, kefir).
3. Home Remedies
Home remedies can provide relief for mild yeast infections or complement medical treatments. However, they are not a substitute for antifungal medications in severe cases.
How They Work:
- Yogurt: Contains live cultures of Lactobacillus, which help restore healthy bacteria and balance pH.
- Coconut Oil: Contains caprylic acid, a natural antifungal that disrupts fungal cell membranes.
- Apple Cider Vinegar: Helps restore the natural pH of the vagina, creating an environment less favorable for yeast growth.
- Garlic: Contains allicin, a compound with antifungal properties that can inhibit Candida growth.
4. Lifestyle and Preventive Measures
While not direct treatments, certain lifestyle changes can help prevent yeast infections and support recovery.
How They Work:
- Good Hygiene: Keeps the affected area clean and dry, reducing the risk of fungal overgrowth.
- Breathable Clothing: Wearing cotton underwear and avoiding tight-fitting clothes reduces moisture, which can promote yeast growth.
- Dietary Changes: Reducing sugar and refined carbs can starve Candida, as it thrives on sugar.
- Hydration: Drinking plenty of water supports overall health and helps flush out toxins.
How Long Do Treatments Take to Work?
- OTC Creams and Suppositories: Most provide relief within 3–7 days, but symptoms often improve within 24–48 hours.
- Oral Antifungals (e.g., Fluconazole): Symptoms typically improve within 24–72 hours after taking the medication.
- Probiotics: May take a few days to weeks to restore balance, depending on the severity of the infection.
- Home Remedies: Relief varies, but improvements may be noticed within a few days.
Why Do Treatments Sometimes Fail?
- Incorrect Diagnosis: Symptoms of yeast infections can mimic other conditions (e.g., bacterial vaginosis or STIs).
- Resistant Strains: Some Candida strains may be resistant to certain antifungals.
- Incomplete Treatment: Stopping treatment early can lead to recurrence.
- Underlying Health Issues: Conditions like diabetes, a weakened immune system, or hormonal imbalances can make infections harder to treat.
How fast do yeast infection treatments work?
The speed at which yeast infection treatments work depends on the type of treatment, the severity of the infection, and individual factors like your overall health. Here’s a breakdown of how quickly you can expect relief from common yeast infection treatments:
1. Over-the-Counter (OTC) Antifungal Creams and Suppositories
- Time to Relief:
- Symptoms like itching and burning often improve within 24–48 hours.
- Most OTC treatments (e.g., Monistat, Gyne-Lotrimin) are designed to clear the infection in 3–7 days, depending on the strength of the product.
- Examples:
- 1-Day Treatment: High-dose creams or suppositories (e.g., Monistat 1) may provide quick relief but can sometimes cause irritation.
- 3-Day or 7-Day Treatments: Lower-dose options are gentler and may be more effective for complete recovery.
2. Oral Antifungal Pills (Prescription)
- Time to Relief:
- Fluconazole (Diflucan): A single-dose pill that typically starts working within 24–72 hours. Most people feel significant relief within 1–2 days.
- For severe or recurrent infections, a second dose may be needed after 72 hours.
- Advantages:
- Convenient and fast-acting.
- Ideal for those who prefer not to use creams or suppositories.
3. Prescription Vaginal Creams
- Time to Relief:
- Symptoms often improve within 2–3 days.
- Full treatment usually takes 7–14 days, depending on the strength of the medication.
- Examples:
- Terconazole (Terazol): A stronger antifungal cream for stubborn infections.
- Nystatin: Often used for oral thrush or skin yeast infections.
4. Probiotics
- Time to Relief:
- Probiotics (oral or vaginal) may take several days to weeks to restore the balance of good bacteria and prevent future infections.
- They are often used as a complementary treatment rather than for immediate relief.
- Examples:
- Lactobacillus rhamnosus and Lactobacillus reuteri: Strains specifically beneficial for vaginal health.
- Probiotic-rich foods like yogurt or kefir can also help.
5. Home Remedies
- Time to Relief:
- Home remedies like yogurt, coconut oil, or apple cider vinegar may provide temporary relief within a few days, but they are not as effective as antifungal medications for clearing infections.
- These remedies are best used as supplements to medical treatments or for mild cases.
Factors That Affect How Fast Treatments Work
- Severity of the Infection: Mild infections may clear up faster than severe or recurrent ones.
- Type of Treatment: Oral medications and high-dose creams often work faster than low-dose creams or home remedies.
- Consistency: Completing the full course of treatment is crucial for preventing recurrence.
- Individual Health: Conditions like diabetes, a weakened immune system, or hormonal imbalances can slow recovery.
When to Expect Full Recovery
- Most yeast infections are fully resolved within 1–2 weeks of starting treatment.
- If symptoms persist beyond this time or recur frequently, consult a healthcare provider to rule out other conditions (e.g., bacterial vaginosis, STIs) or resistant strains of yeast.
Tips for Faster Relief
- Follow Instructions: Use the treatment as directed, even if symptoms improve before the course is complete.
- Avoid Irritants: Steer clear of scented products, douches, or tight-fitting clothing.
- Maintain Hygiene: Keep the affected area clean and dry.
- Stay Hydrated: Drink plenty of water to support overall health.

Are there any side effects or safety concerns for yeast infection treatments?
Yes, yeast infection treatments, like any medications or remedies, can have side effects or safety concerns. While most people tolerate these treatments well, it’s important to be aware of potential risks and take precautions, especially if you have underlying health conditions or are pregnant. Here’s a detailed look at the side effects and safety concerns associated with common yeast infection treatments:
1. Over-the-Counter (OTC) Antifungal Creams and Suppositories
These are generally safe but can cause mild side effects in some people.
- Common Side Effects:
- Vaginal burning, itching, or irritation.
- Redness or swelling at the application site.
- Mild abdominal pain or cramping.
- Safety Concerns:
- Avoid using these products if you are allergic to any of the ingredients.
- Do not use tampons or douches while using vaginal creams or suppositories, as they can reduce the effectiveness of the treatment.
- If symptoms worsen or persist after treatment, consult a healthcare provider.
2. Oral Antifungal Pills (e.g., Fluconazole/Diflucan)
Oral medications are effective but can have more systemic side effects compared to topical treatments.
- Common Side Effects:
- Nausea, vomiting, or stomach pain.
- Headache or dizziness.
- Diarrhea or changes in taste.
- Serious Side Effects (Rare):
- Liver problems (e.g., jaundice, dark urine, or severe fatigue).
- Allergic reactions (e.g., rash, swelling, or difficulty breathing).
- Irregular heartbeat or severe dizziness.
- Safety Concerns:
- Inform your doctor if you have liver or kidney disease, as fluconazole can affect these organs.
- Avoid alcohol while taking oral antifungals, as it can increase the risk of liver damage.
- Pregnant women should consult a doctor before using oral antifungals, as they may not be safe during pregnancy.
3. Prescription Vaginal Creams
Prescription-strength creams are stronger than OTC options and may have similar or more pronounced side effects.
- Common Side Effects:
- Vaginal irritation, burning, or itching.
- Headache or stomach discomfort.
- Safety Concerns:
- Use as directed by your healthcare provider.
- Avoid sexual intercourse during treatment, as some creams can weaken latex condoms or diaphragms.
- Inform your doctor if you experience severe irritation or allergic reactions.
4. Probiotics
Probiotics are generally safe but can cause mild side effects in some individuals.
- Common Side Effects:
- Bloating or gas.
- Mild stomach upset.
- Safety Concerns:
- Choose high-quality probiotic supplements from reputable brands.
- People with weakened immune systems or serious medical conditions should consult a doctor before using probiotics.
- Vaginal probiotic suppositories may cause temporary irritation or discharge.
5. Home Remedies
While natural, home remedies can still cause side effects or safety issues if not used properly.
- Yogurt:
- Side Effects: Rare, but some people may experience irritation or allergic reactions.
- Safety Concerns: Use only plain, unsweetened yogurt with live cultures. Avoid flavored or sweetened varieties.
- Coconut Oil:
- Side Effects: Rare, but may cause irritation in some individuals.
- Safety Concerns: Avoid using with latex condoms, as oil can break down latex.
- Apple Cider Vinegar:
- Side Effects: Can cause burning or irritation if not properly diluted.
- Safety Concerns: Always dilute with water before use (e.g., 1–2 tablespoons per cup of water).
- Garlic:
- Side Effects: May cause irritation or allergic reactions.
- Safety Concerns: Use with caution; inserting garlic vaginally can sometimes cause burns or infections.
Special Considerations
- Pregnancy: Pregnant women should avoid oral antifungals and consult a doctor before using any yeast infection treatment. Some OTC creams (e.g., clotrimazole) are considered safe during pregnancy, but always check with a healthcare provider.
- Recurrent Infections: If you experience frequent yeast infections (more than 4 per year), consult a doctor to rule out underlying conditions like diabetes or immune system issues.
- Allergies: If you have a history of allergic reactions to antifungal medications or natural ingredients, proceed with caution and consult a doctor.
When to Seek Medical Attention
- If symptoms worsen or do not improve after completing treatment.
- If you experience severe side effects like difficulty breathing, swelling, or severe abdominal pain.
- If you suspect you may have a different condition (e.g., bacterial vaginosis or an STI).
fastinfosearch site provides the best information
Suggested content:





No comment